- 1Who Can Get Dermatitis Herpetiformis?
- 2What Are the Causes of Dermatitis Herpetiformis?
- 3What Are the Clinical Features of Dermatitis Herpetiformis?
- 4What Are the Symptoms of Dermatitis Herpetiformis?
- 5What Are the Complications of Dermatitis Herpetiformis?
- 6How to Diagnose Dermatitis Herpetiformis?
- 7How to Treat Dermatitis Herpetiformis?
- 8When to Consult a Healthcare Provider for Dermatitis Herpetiformis?
Introduction:
Dermatitis herpetiformis, also known as Duhring-Brocq disease, is characterized by an intensely itchy, chronic papulovesicular eruption usually distributed symmetrically on the extensor surfaces. After its presentation, the condition persists indefinitely in varying severity. The prevalence varies from 10 to 39 per 100,000 persons.
Who Can Get Dermatitis Herpetiformis?
Dermatitis herpetiformis occurs more commonly in males than females in the ratio of 2:1 in the second, third, or fourth decades. There may be a family history of autoimmune diseases such as pernicious anemia, thyroid disorders, type 1 diabetes, Addison disease, and alopecia. Genetic predisposition with human leukocyte antigen is also found.
What Are the Causes of Dermatitis Herpetiformis?
Gluten is a protein found in wheat, barley, and rye, which plays a critical role in the pathogenesis of dermatitis herpetiformis. IgA (Immunoglobulin A) antibodies formed against this protein in the predisposed individuals are thought to cross-react with certain antigens of the dermal-epidermal junction, leading to the clinical expression of the disease. Most patients with this condition probably have some gastrointestinal abnormality, such as diarrhea, weight loss, tiredness, and abdominal discomfort, similar to celiac disease. The patients with coeliac disease have concurrent dermatitis herpetiformis and tend to have more intestinal pathology.
What Are the Clinical Features of Dermatitis Herpetiformis?
-
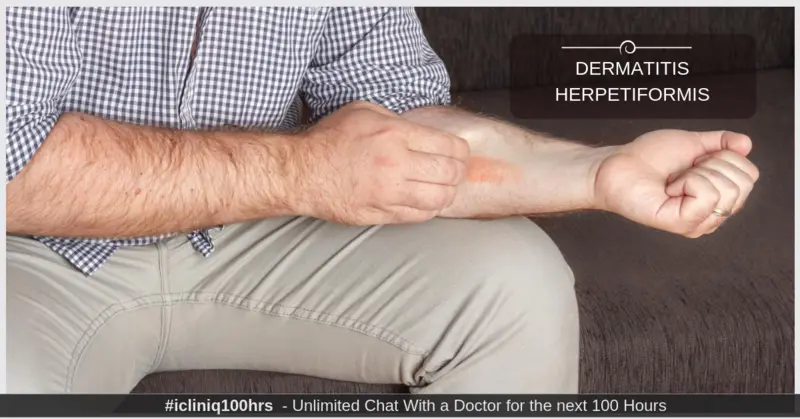
Dermatitis herpetiformis is either an erythematous papule such as a urticaria-like plaque or, most commonly, a vesicle. It initially appears as petechiae, which progresses further to form papular lesions.
-
The patchy lesion can sometimes resemble lesions of other inflammatory skin conditions such as dermatitis, scabies, etc.
-
The lesions are usually itchy and located symmetrically on the elbows, knees, shoulders, lower back, and buttocks.
-
The face and facial hairline may also be involved.
-
They often appear in clusters, and large bulla is infrequent.
-
The lesion resolves and leaves post-inflammatory hyperpigmentation or hypopigmentation.
What Are the Symptoms of Dermatitis Herpetiformis?
Some common symptoms are:
-
Skin Issues: This is the most common symptom of this condition, affecting the skin. Discolored bumps and itchy and burning blisters may be present.
-
Oral Issues: This condition can also affect the enamel of the tooth. There may be pitting, discoloration, or grooves present on the tooth. In rare conditions, canker sores may be present.
-
Gastrointestinal Issues: Most people with this condition are sensitive to gluten and suffer from celiac issues. This condition can damage the small intestine.
What Are the Complications of Dermatitis Herpetiformis?
In Gastrointestinal Tract:
-
Steatorrhea (excess stool fat) and D-xylose malabsorption are observed in 20 % to 33 % of patients.
-
Iron and folate malabsorption leading to anemia is rare.
-
DH patients also have an increased incidence of achlorhydria (absence of hydrochloric acid in gastric secretions) and atrophic gastritis (inflammation of gastric mucosa).
Malignancy: There is an increased frequency of gastrointestinal lymphomas and non-Hodgkin’s lymphoma in dermatitis herpetiformis patients.
Neurological Problems: They can have ataxia (loss of balance), epilepsy (seizures), and polyneuropathy (damage to the peripheral nerves).
Heart Problems: Cardiomyopathy (disease of the heart muscle) and pericarditis (inflammation of the sac surrounding the heart) can occur.
Autoimmune Diseases: These patients also have a high incidence of autoimmune diseases, such as:
-
Insulin-dependent diabetes mellitus.
-
Autoimmune thyroid disease.
-
Pernicious anemia.
-
Addison's disease (insufficient production of certain hormones by the adrenal glands).
-
Lupus erythematosus (the immune system attacks its own tissues, causing inflammation).
-
Vitiligo (a long-term immune condition that causes skin areas to lose pigment).
-
Myasthenia gravis (weakness of voluntary muscles).
-
Scleroderma (chronic hardening and tightening of the connective tissues and skin).
-
Sarcoidosis (immune system to react improperly and develop granulomas).
How to Diagnose Dermatitis Herpetiformis?
Skin Biopsy: A skin biopsy is a confirmatory test for diagnosing dermatitis herpetiformis. The histologic features include:
-
Subepidermal Blisters: Blisters that are placed beneath the layers of skin.
-
White Blood Cells: Neutrophils and eosinophils are present in the dermal layer.
-
Iga Deposits: IgA deposits are visible in the dermal layer through direct immunofluorescence.
Tests for Nutritional Deficiencies: Patients with coeliac disease are screened for nutritional deficiencies, such as complete blood count, iron, zinc, vitamin B12, folate levels, serum calcium levels, thyroid function tests, and liver function tests. Iron and folic acid levels are evaluated as mild anemia, possibly due to malabsorption associated with gluten-sensitive enteropathy. Thyroid function tests are recommended as thyroid diseases and dermatitis herpetiformis are associated with each other.
Autoantibody Tests: The specific tests include IgA anti-endosomal antibodies, IgA tissue transglutaminase antibody, IgA and IgG (Immunoglobulin G) gliadin assay, and total IgA level.
Small Intestinal Biopsy: The patients showing abnormal results in blood tests are subjected to intestinal biopsy to confirm gluten-sensitive enteropathy. The histology shows atrophy of the bowel, which indicates the flattening of the intestinal lining.
How to Treat Dermatitis Herpetiformis?
-
Dapsone: Dapsone is the drug of choice for dermatitis herpetiformis, which is usually 100 to 150 mg daily. Occasionally, patients will require double this dose. There is prompt relief of symptoms, and no new lesions erupt after one to two days of therapy. However, the patients must be on a minimal dose of Dapsone (sometimes as little as 25 mg on alternate days) because the disease activity increases sharply on cessation of treatment. If the patient is allergic or intolerant to Dapsone, ultra-potent topical steroids, systemic steroids, Sulfapyridine, and Rituximab can be taken.
-
Gluten-Free Diet: The intestinal lesions respond well to a gluten-free diet. Strict adherence to this diet will reduce the requirement for medication in most patients. It further improves gluten-sensitive enteropathy, nutrition, and bone density. In addition, the diet reduces the risk of developing autoimmune diseases. However, highly motivated individuals can adhere to this diet. Thus, do not take itchiness lightly, as it is common in most skin diseases.
How Long Will a Person Have Dermatitis Herpetiformis?
Dermatitis herpetiformis can persist lifelong unless diet modification is established.
Is Dermatitis Herpetiformis Contagious?
Dermatitis herpetiformis is non-contagious, like any other type of dermatitis. It cannot spread from one person to another.
When to Consult a Healthcare Provider for Dermatitis Herpetiformis?
If the person feels any symptoms of dermatitis herpetiformis, it is good to report it to the healthcare provider immediately. The itchy feeling of the condition can affect the quality of life. Try consulting a dermatologist initially who would recommend some diagnostic tests. And if the person has a nutritional deficiency, the nutritionist will follow up. Getting identified and treated earlier is the best choice.
Conclusion:
Living with visible bumps and blisters is more complex than adapting to a new diet. Therefore, whenever a person gets tempted by their favorite food, remember it is worth avoiding them rather than suffering from those itchy blisters. Do not modify the diet and take medicines without consulting a doctor. Consult the specialist and take necessary precautions with their consent. Stay gluten-free, stay dermatitis herpetiformis-free.