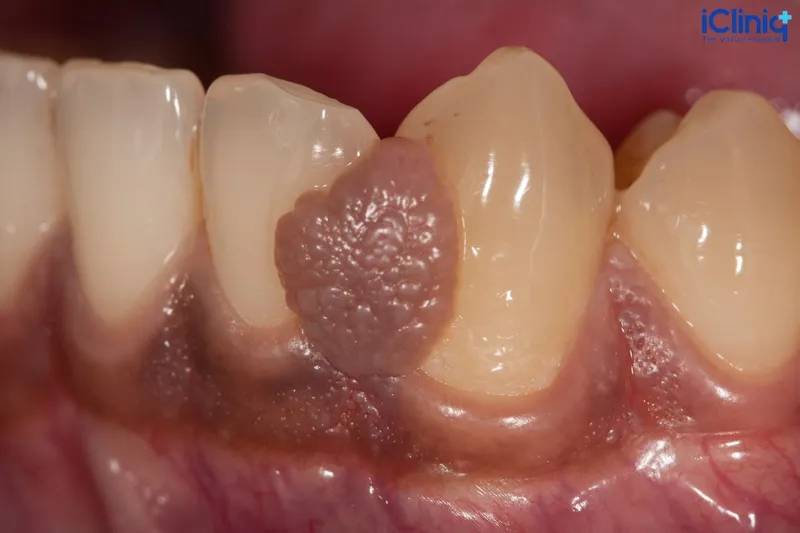
What Is Oral Fibroma?
Oral fibromas are benign growths seen in the oral cavity at the site of irritation. Other names, such as reactive hyperplasia, traumatic fibroma, focal intraoral fibrous hyperplasia, oral polyp, or fibrous nodule, are more commonly used. The shape, size, structure, and consistency may vary depending on the composition of the fibroma. Oral fibromas can also be pedunculated; a stalk might be evident that connects the outgrowth of tissue to the underlying tissue. However, not all oral fibromas are pedunculated.
What Causes Oral Fibroma and Who Is More Commonly Affected by Oral Fibromas?
As the name suggests, traumatic fibroma, or oral fibroma, is found intraorally in the tongue, inner surfaces of the cheeks, or gums. Any constant localized trauma can lead to tissue outgrowth, hence the name.
Older people are more commonly affected by oral fibroma, and there is no gender predilection seen. That means both men and women are equally affected by oral fibromas.
-
Wearing an ill-fitting denture can cause constant irritation to the underlying tissues, leading to traumatic fibroma.
-
Any compulsive habits like biting the cheek or lips may cause traumatic fibroma.
-
Dental prostheses like crowns and veneers that do not fit properly might irritate the underlying and adjacent tissues, leading to oral fibromas.
-
Ill-fitting orthodontic brackets with sharp edges that cause constant irritation can lead to oral fibromas in younger adults and children.
-
When a person has teeth out of the arch that interferes with the inner cheek while biting, it may lead to oral fibromas.
How Would a Person Describe the Appearance of an Oral Fibroma?
-
Common Location: It is frequently located on the gums, inside the cheek, on the tongue, or along the inner lining of the mouth.
-
Appearance and Sensation: It typically appears as a dense, solid mass, often exhibiting a pink or gum-like coloration. When touched, it may feel like a firm lump or dome.
-
Variable in Size: Can vary in size from small polyps to larger lesions.
-
Association With Ulcers: Occasionally, they might be linked with mouth ulcers or lesions.
-
Possible Association With Stress: There is a suggestion that mechanical pressure, such as frequent biting or sustained pressure, could contribute to the formation of oral fibromas.
-
Differentiation from Other Tumors: Distinguishing oral fibroma from other oral tumors, like neurofibroma, is crucial and can be achieved through clinical assessments and, when necessary, biopsies.
What Are the Signs and Symptoms of Oral Fibroma?
The dentist can easily identify oral fibroma based on the presence of the following signs and symptoms,
-
Oral fibroma, most commonly, does not cause any symptoms.
-
Oral fibroma presents in the mouth at the site of constant trauma as a firm nodule or growth.
-
The growth mostly remains in the color of the surrounding tissues; however, sometimes, constant trauma and bleeding of the nodule may change the color to bright red or pink.
-
An oral fibroma can be seen with a stalk connecting the growth to the underlying tissue, and this condition is called pedunculated oral fibroma.
How Can an Oral Fibroma Be Diagnosed?
The dentist can easily diagnose oral fibromas or traumatic fibromas by asking specific questions like,
-
The dentist will check intraorally for any ill-fitting dental prosthesis or check for any teeth out of the arch that might injure the soft tissues during occlusion.
-
A biopsy might be performed to exclude other conditions like Cowden syndrome, tuberous sclerosis, familial fibromatosis, and fibrotic papillary hyperplasia of the palate.
How to Treat Oral Fibroma?
The most common oral or traumatic fibroma treatment is removing the growth locally. This removal of oral fibroma can be done in two ways, namely,
-
Surgical removal of oral fibroma under local anesthesia using a scalpel.
-
Laser removal of oral fibroma.
Laser removal is the most recent method of removing oral fibroma because it minimizes the scarring after removal. The removal of oral fibroma using a scalpel might need a suture, and it might lead to permanent scarring of the tissues. Also, the conventional method of removing oral fibromas using scalpels might lead to unwanted and undesirable blood loss.
-
The removed tissue is then sent for biopsy to rule out the presence of other conditions that mimic oral fibromas.
-
The next and most crucial step in managing oral fibroma or traumatic fibroma is to remove the presence of any object or ill-fitting prosthesis that causes oral fibroma.
-
The sharp edges of the tooth can be smoothed to avoid future trauma.
-
Orthodontic treatments can correct any tooth that is misaligned.
-
Sharp or rough edges of any dental crowns or fillings should be smoothed.
-
Ill-fitting dentures should be redone, or they should be trimmed and polished to fit perfectly.
-
Any habits like cheek biting should be ceased by proper counseling.
What Measures Can Individuals Take to Reduce the Risk of Developing Fibromas?
Preventing oral fibromas involves minimizing chronic irritation to the mouth. This can be achieved by adopting healthy oral habits and being mindful of behaviors that may lead to tissue trauma. For instance, individuals should avoid habitual cheek biting or chewing on hard objects like pens or fingernails. Maintaining good oral hygiene, including regular brushing and flossing, can help prevent irritation and reduce the risk of developing fibromas.
Additionally, addressing any dental issues, such as ill-fitting dental appliances, can prevent repetitive trauma to the oral tissues. Being conscious of stress-related habits like clenching or grinding teeth and seeking appropriate management strategies can also be beneficial.
Regular dental check-ups allow for early detection and management of potential oral lesions, further contributing to prevention efforts. Awareness, healthy habits, and prompt dental care can help individuals minimize the risk of developing oral fibromas.
Conclusion:
Oral fibroma is a benign condition, and it does not become cancer. Proper diagnosis and treatment are necessary to remove oral fibroma. Also, any sharp edges, ill-fitting dentures, or habits that cause constant tissue trauma must be corrected to avoid future injury, which might lead to recurrent oral fibromas. Any painless growth in the oral cavity need not cause the person stress, as not all growths are considered cancer. They can be as simple as a traumatic fibroma caused by an ill-fitting denture, orthodontic brackets, or the compulsive cheek-biting habit that might have developed the traumatic fibroma. If the person notices any intraoral growth associated with trauma, consult the dentist to get it diagnosed and remove it as soon as possible.